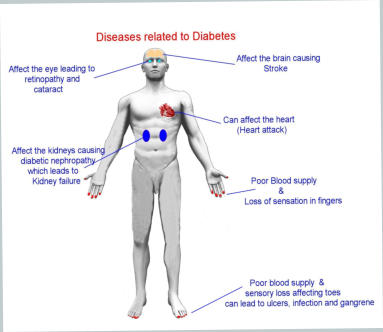
Blood Sugar and Diabetes Mellitus.
Diabetes has now become a major health problem worldwide.
Research suggests that in another 10 years 75% of the world adult
population will suffer from diabetes. It used to be a disease of the
western population but with increasing wealth in India and China, it is
predicted that it will soon become a major problem in these two
countries.
Sugar in our blood is essential for life, as glucose is the primary
source of energy for all living cells in the body. Glucose is absorbed
and transported from the intestine to the cells. With the help of the
hormone insulin the cells use the sugar for their metabolism. What is
not used by the cells is stored in organs like the liver and muscle. The
body tightly regulates the blood sugar level
It is remarkable that despite widely variable intervals between meals
or the occasional consumption of meals with excessive sugar, the
level of blood sugar remains within the normal range. The delicate
balance is done through hormones. Insulin produced by the body
helps the cells to use the sugar. The blood sugar level is lowest in the morning before you start eating and rises 1 or 2 hours after
every meal to its highest level. In a normal individual the blood sugar when you are fasting ranges from 70 mg/dl to 120 mg/dl (4 to
6.5 mmol/L) with occasional slightly lower or higher values.
When blood sugar levels drop too low (hypoglycaemia) a person feels lethargic with diminished mental function, irritability and
weakness of muscles. Sometimes the person may develop fits. It can lead to unconsciousness and can be fatal. Hypoglycaemia is
more dangerous than hyperglycaemia (excess sugar).
In diabetes mellitus the cells are unable to use the circulating sugar effectively because of lack of insulin or because very little insulin
is produced or the cells are resistant to using insulin.
When no insulin or very little insulin is produced you develop type 1 diabetes. When reduced amount of insulin is produced or the
cells become resistant to use the insulin you develop type 2 diabetes. Type 1 diabetics will therefore require insulin injections,
whereas type 2 diabetes can often be managed with dietary and lifestyle changes with or without a tablet.
How do we know whether it is type 1 or type 2 diabetes?
Type II diabetes is more common than Type I diabetes and it usually occurs in older people. However it may only be picked up
during a routine medical check-up as patients may not have any symptom to start with. There are a number of diagnostic tools for
differentiating type 1 from type 2 diabetes. As type 1 diabetes is an autoimmune disease anti-islet cell antibodies and anti-insulin
antibodies may be detected.
Physicians distinguish type 1 and type 2 diabetes by performing a blood test called the C-Peptide Test. If the C-Peptide is negative it
means that the person is not making insulin and that they have type 1 diabetes and if the C-Peptide is positive it means that the
person is making insulin and that they have type 2 diabetes.
Symptoms
Some symptoms are common to both type 1 and type 2 diabetes. They are:
•
Excessive thirst
•
Passing urine frequently
•
Feeling tired and light headed
•
Loss of weight.
•
Symptoms of Type I diabetes may come on suddenly and can be severe.
In Type 2 Diabetes in addition to the above, after a while the person may also notice –